
Sentinel events occur when a patient is seriously injured (permanently or temporary) or causes death, happening outside the predictable course of the patient’s disease process.
Sentinel events are debilitating to both patients and healthcare providers involved in the event. The Joint Commission works closely with organizations to address sentinel events and to prevent them from occurring in the first place.
CHT is a national leader providing support to healthcare facilities in identifying and developing compliance programs regarding their medical gas needs and environmental monitoring to protect patients and employees. We understand the contributing factors and actions facilities can take to reduce the risk of these events.
Based on our experience, we thought we would address sentinel events with examples, statistics, and a 5-step process of what to do when and if a sentinel event occurs in your facility.
In addition, one of the requirements and concerns as a healthcare facility manager is the ventilation in your care areas. Because of the airflow standards, equipment must meet high ventilation rates and filtration requirements . . .

What are Examples of Sentinel Events?
The events are named "sentinel" because they signal the need for immediate investigation and response.
As of Jan. 1, 2022, The Joint Commission’s Office of Quality and Patient Safety (OQPS) revised its definition of a sentinel event and clarified some of the event-specific examples in the Sentinel Event Policy.
OQPS revised the definition to clarify the differences between severe harm (which may or may not be permanent) and permanent harm (regardless of severity).
The revised definitions include:
- Sentinel event: A patient safety event (not primarily related to the natural course of the [patient’s] illness or underlying condition) that reaches a [patient] and results in death, severe harm (regardless of the duration of harm), or permanent harm (regardless of the severity of harm).
- Severe harm: An event or condition that reaches the individual, resulting in life-threatening bodily injury (including pain or disfigurement) that interferes with or results in loss of functional ability or quality of life that requires continuous physiological monitoring or a surgery, invasive procedure, or treatment to resolve the condition.
- Permanent harm: An event or condition that reaches the individual, resulting in any level of harm that permanently alters and/or affects an individual’s baseline.
From a facility's perspective, an example of a sentinel event could be a fall event or the failure of some equipment that is part of the regular building function. This could include the failure of room outlets to provide oxygen or failure of inlets to provide sufficient vacuum to a patient.
According to the Joint Commission, the most common cause of sentinel events in healthcare includes unintended retention of a foreign object, fall-related events, and performing procedures on the wrong patient. Others include delay in treatment, medication error, and fire-related events.
Falls resulting in injury are a prevalent safety problem. The Joint Commission states,
"A fall may be described as an unintentional change in position coming to rest on the ground, floor, or onto the next lower surface (e.g., onto a bed, chair, or bedside mat). The fall may be witnessed, reported by a patient, an observer, or identified when the patient is found on the floor or ground. Falls include any fall whether it occurred at home, out in the community, in an acute hospital, or ambulatory setting." — The Joint Commission, Does the Joint Commission provide an official definition of a patient 'fall' or does each organization need to define it?
Most Frequently Reported Sentinel Events (1st Half of 2021 Statistics)
Through the first six months of 2021, The Joint Commission reviewed 569 sentinel events. The majority of events—516 total or 91%—were self-reported by an accredited or certified organization.
The remaining 53 sentinel events were reported either by patients (or their families) or employees (current or former) of the organization.
Sentinel event statistics for the first half of 2021 covers 16,695 incidents reported from 1995 through June 30, 2021. These events affected a total of 14,105 patients (as multiple patients may be affected by a single event):
Sentinel Events Led To . . .
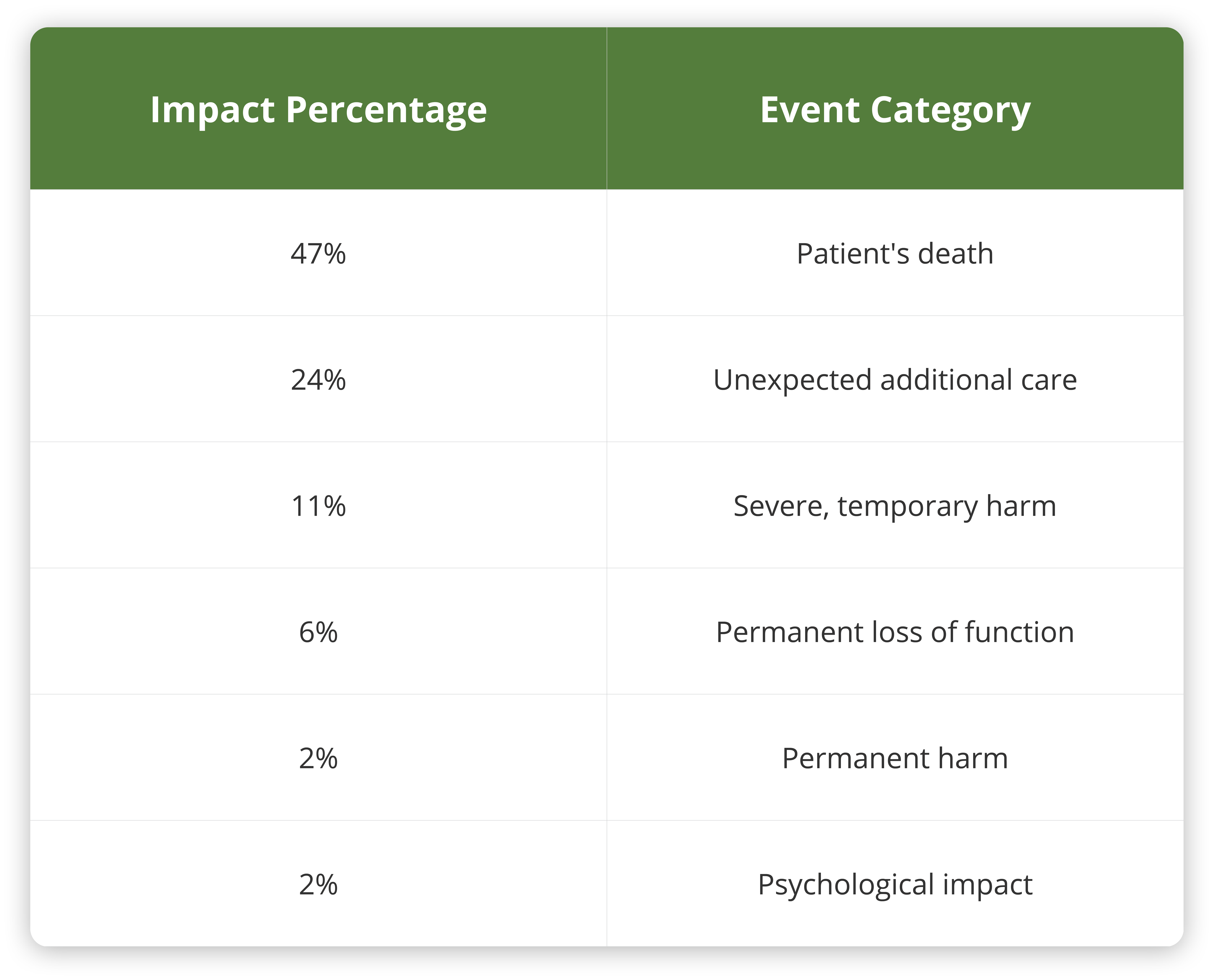
Source: The Joint Commission, Sentinel event data released for the first six months of 2021
- 47% of sentinel events led to a patient’s death.
- 24% led to unexpected additional care.
- 11% led to severe, temporary harm.
- 6% led to permanent loss of function.
- 2% led to permanent harm.
- 2% led to a psychological impact.
Note: An estimated fewer than 2% of all sentinel events are reported to The Joint Commission.
Facing a Sentinel Event Head-on (What to Do When an Event Occurs)
The Joint Commission offers a five-step process of what to do next.
"Take 5 With the Joint Commission: What to do when a sentinel event occurs" features pointers from Patricia McColl, RN, a patient safety specialist at The Joint Commission's office of quality monitoring and patient safety, on what to do when a sentinel event occurs at your organization.
Step 1: Secure the situation - Ensure the patient and staff's well-being is being cared for.
Step 2: Preserve anything that might be helpful in the investigation - for example, equipment, tubing, medications.
Step 3: Disclose the situation and relevant information to the patient or caregiver.
Step 4: Provide support for the patient, family, and staff.
Step 5: Follow The Joint Commission's reporting and root-cause analysis requirements, detailed in the organization's accreditation manual. A root-cause analysis should be performed as soon as possible after the sentinel event.
The five-step process helps improve care, treatment services and prevent future events.
It emphasizes factors and underlying causes, conditions, etc., rather than individual performance.
Resource:
Take 5 Podcast: What to Do When a Sentinel Event Occurs
What Are the Requirements of TJC for Sentinel Events?
The Joint Commission has an extensive program to identify and record these sentinel events so they will be remedied and others in healthcare can be alerted to avoid similar problems.
Their regimen requires:
- A formalized team response that stabilizes the patient, discloses the event to the patient and family and provides support for the family as well as staff involved in the event
- Notification of hospital leadership
- Immediate investigation
Patient Safety Event versus Sentinel Event
A patient safety event is an event, incident, or condition that could have resulted or did result in harm to a patient. This event can be, but is not necessarily, the result of a flawed system or process design, a system breakdown, equipment failure, or human error. Patient safety events include adverse events, no-harm events, close calls, and hazardous conditions.
Each hospital must have a detailed plan communicated to all staff that defines patient safety, including what events are considered sentinel and what incidents are patient safety events.
The hospital CEO is responsible to TJC to provide these plans and to show that action has been taken to:
- Explain why the incident happened
- Who and what equipment was involved
- How the accident or event will be avoided in the future
Likewise, the plan should define:
- Who is responsible for fixing the equipment or procedure
- When the fix is complete
- How this planned repair or procedure change will avoid future events
- How the TJC and the patients can be assured the fix will be enforced
Closing thoughts
Organizations are reporting sentinel events to help identify contributing factors and actions healthcare facilities can take to reduce risk and improve quality.
Events are rare because facilities do their best to provide safe and effective care for patients, but accidents and anomalies happen. Healthcare facilities and organizations are taking an integrated approach to maintain and exceed patient safety.
CHT partners with healthcare facilities to provide the tools and expertise needed to comply with The Joint Commission, OSHA, NIOSH, AHA, and other governing authorities.
With the ability to provide a wide range of engineering, maintenance, environmental monitoring, and consulting services, CHT is on the leading edge of a constantly evolving healthcare industry. Combining knowledge, experience, convenience, and effectiveness brings our healthcare partners world-class technology and service that gives them peace of mind.
This is the value of regular equipment inspections and testing to ensure the assets in your buildings are working correctly, providing the best outcomes to patients, staff, and TJC surveyors.




