
Are you struggling with Medical Gas Compliance?
CHT offers medical gas services to help you reach your compliance goals. To help you navigate through these challenges, start with a free 30-minute discovery call.

Positive Versus Negative Pressure Rooms
Positive pressure rooms have a higher pressure inside the treated room than that of the neighboring environment. In this way, any airborne particle that originates in the room will be filtered. In contrast, negative pressure rooms have lower air pressure. This traps and keeps potentially harmful particles within the room.
Purpose of Negative Pressure Rooms
A negative pressure room in a hospital is used to contain airborne contaminants within the room. Viruses, bacteria, fungi, yeasts, molds, pollens, gases, VOC’s (volatile organic compounds), small particles and chemicals are part of larger list of airborne pathogens you can find in a hospital.
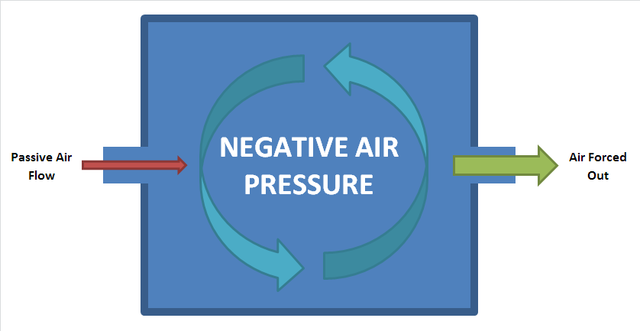
Image credit: By Rrobotto - Own work, Negative air pressure CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=56580980
Isolation rooms are negatively pressurized with respect to adjacent areas to prevent airborne contaminants from drifting to other areas and contaminating patients, staff and sterile equipment.
Rooms to Negatively Pressurize
Rooms that should be negatively pressurized according to the 2018 FGI Guidelines ANSI/ASHRAE/ASHE Standard 170-2017 include, but are not limited to:
- Emergency Department Public Waiting Areas
- Emergency Department Decontamination
- Radiology Waiting Rooms
- Triage
- Bathrooms
- Airborne Infection Isolation (AII) Rooms
- Most Laboratory Work Areas
- Autopsy Rooms
- Soiled Workrooms or Soiled Holding Rooms
- Soiled or Decontamination Rooms in Sterile Processing Department
- Soiled Linen Sorting and Storage
- Janitors’ Closets
Negative Pressure in Isolation Rooms
A negative pressure isolation room is commonly used for patients with airborne infections. Although COVID-19 is currently not considered to be an airborne disease, according to the CDC, a patient known to have contracted the coronavirus can spread it person-to-person. This means between people who are in close contact with one another (within about 6 feet), or through respiratory droplets produced when an infected person coughs or sneezes.
Positive Pressure Rooms
Positive pressure can be used in rooms adjacent to a negative pressure room. This means that the air pressure inside a positive pressure room is greater than the pressure outside of it which is achieved by pumping in filtered, clean air. The purpose of positive pressure is to ensure that airborne pathogens do not contaminate the patient or supplies in that room. For example, positive pressure could be used in an operating room to protect the patient and sterile medical and surgical supplies. Positively pressured rooms are typically considered the cleanest rooms in the hospital.
Unbalanced Pressure Checklist
To prevent unbalanced pressure, routine checks should be made. Here's a short list of where you should start...
- Monitor the supply and exhaust rates for the room.
- Check that supply and exhaust fans are operating properly.
- Check for blockages of supply diffusers and return grilles within the room; occupants may block them in an effort to improve their thermal comfort.
- Check performance of fume hoods and biological safety cabinets within the room and in adjacent rooms. Poor performance of these units affects air balance within nearby rooms.
- Monitor all pressure systems after any renovation. Renovations may alter the HVAC system in a manner that impacts the air balance among nearby rooms.
Creating Negatively and Positively Pressured Rooms
Most hospital HVAC duct systems can be reworked to accommodate special air pressures in fixed rooms. Since it can be expensive to remodel to create negatively and positively pressured rooms here are a couple germ fighting options.
The first approach is killing the pathogens, which requires a relatively high dose of ultraviolet (UV) radiation installed into HVAC systems, but the cost of this is considerable.
The other option is a commercial one. NQ Industries Inc. has developed products for medical application in contaminated environments including mobile Ultraviolet-HEPA-Carbon-Photocatalysis air purification systems.
Conclusion
When rooms are not properly pressurized (negative or positive), airborne contaminants can escape putting the health of patients, staff, and visitors at risk.
This has never been more important than right now. No matter what system is used, the need for properly functioning negative and positive pressurized rooms in the hospital is well documented. Together, we can navigate these trying times and provide positive patient outcomes.
CHT offers medical gas services to help you reach your compliance goals. To help you navigate through these challenges, we offer a free 30-minute discovery call.




